How Health Systems and Communities Can Measure Progress in Health Equity
- Genesis Health Consulting

- Nov 28, 2018
- 5 min read
Throughout November, Genesis Health Consulting blog posts focused on health equity: why it’s a critical issue for our time; the unique opportunity and accountability of hospitals and health systems to improve health equity; and why partnering with communities is more likely to creating meaningful and sustainable change.
Today, we close this series with a discussion of how to measure progress toward improving health equity. Examining data through a health equity lens is often new territory for health systems and communities. Frequently, additional perspectives, data, expertise and partnerships are needed to ensure that measurement is designed to assess the heterogeneous drivers of health disparities and health equity.
In this article, we’ll walk through common resource needs and challenges in designing health equity measurement, and profile different types and sources of data that can inform measurement selection.
Resources
It’s helpful to begin with an understanding of how different communities experience health disparities and which community members are most vulnerable to these disparities. To answer those questions, you’ll need to test your hypotheses against a wide range of data sources that reflect local experiences. The specific environmental, cultural, social and political conditions in which people live have a disproportionate effect on health and wellbeing. And these conditions can swing wildly based on neighborhood of residence, annual earnings, race, gender, sexuality, age, and the like. Data sources should be organized to enable analysts to test hypotheses about local drivers of health disparities, and to compare experience in equity across different populations.
Reviewing publicly-available data sets can be a helpful starting point when assessing local experiences and outcomes related to health equity. Because these data sources are designed for public use, data is presented at the population-level. It is likely that more specific, local data is available in your community. We strongly urge researchers to seek these local sources to complement other public data sets. (Scroll down to find a list of well-regarded public data sets that can inform health equity measurement.) Finally, training in epidemiological research, public health or public policy research can be a helpful asset when selecting data sets, forming questions, and conducting analysis.
Partnerships are another key enabler of this work. Consider strategic partnerships with local service organizations like food pantries, child welfare agencies, public education systems or 211 agencies that will bring new data sources to your analysis. Partnerships with think tanks, academic institutions or community organizations can provide helpful insight and collaboration from subject matter experts in health equity and analytics. Partnerships with health care organizations and health insurance companies may facilitate access to medical records and claims data, allowing measurement to reach into questions of impact, outcomes, or cost. Perhaps most importantly, partnerships with resident organizations and community leadership groups will bring a critical check on how to design and execute a measurement strategy. For example, do the data sources and questions of the data resonate with the lived experience of community residents? Are you measuring what matters to them?
Challenges
No one data set or organization can tell the whole story of child health in a community. One challenge in health equity measurement is the ability to link disparate data sets around a common identifier. This may be due to data being collected anonymously, differences in how key variables are defined, privacy restrictions, and level of detail provided (e.g., census tracts vs. Congressional district vs. county-level data). Most health equity measurement initiatives maximize the data available to them, and accept the limitations therein. There is a natural tipping point within each project where incorporating additional data has a diminishing return. It is up to the leadership of the project to determine when that point has been reached.
Of the challenges mentioned, only privacy restrictions afford some room for negotiation in the near term. (Data collection methodology, definitions and granularity are decisions made at the beginning of building a data set, which is most often well before the data set is referenced for measurement strategies.) Some communities have successfully addressed privacy restrictions by establishing an independent, representative body to collect, match, and analyze data from various public and private entities like schools, police departments, housing, etc. This is no small lift, and should be viewed as a multi-year investment.
Researchers may also face challenges in managing expectations of different stakeholders when designing health equity measures. The drivers of health inequities are numerous and interconnected. It is extraordinarily difficult to isolate the impact of specific variables and interventions in a dynamic environment, particularly when the data sources used for measures are designed for public or general use. It is important to understand and manage stakeholder expectations early by discussing how your measurement strategy will address these challenges.
Finally, it may be that a community needs to design new health equity indicators, including a strategy for where the data will be collected and tracked over time. Community Health Needs Assessments (CHNA) are a community-specific tool that can provide additional insight into community priorities and provide a mechanism to collect community specific indicators of health equity through shared ownership and accountability. Non-for-profit hospitals and health systems are required to conduct a CHNA every three years per the Affordable Care Act. The Centers for Disease Control website has a variety of resources for health systems to use in implementing a truly collaborative CHNA process. The American Public Health Association and Institute for Health Improvement also offer guidance on measuring health equity.
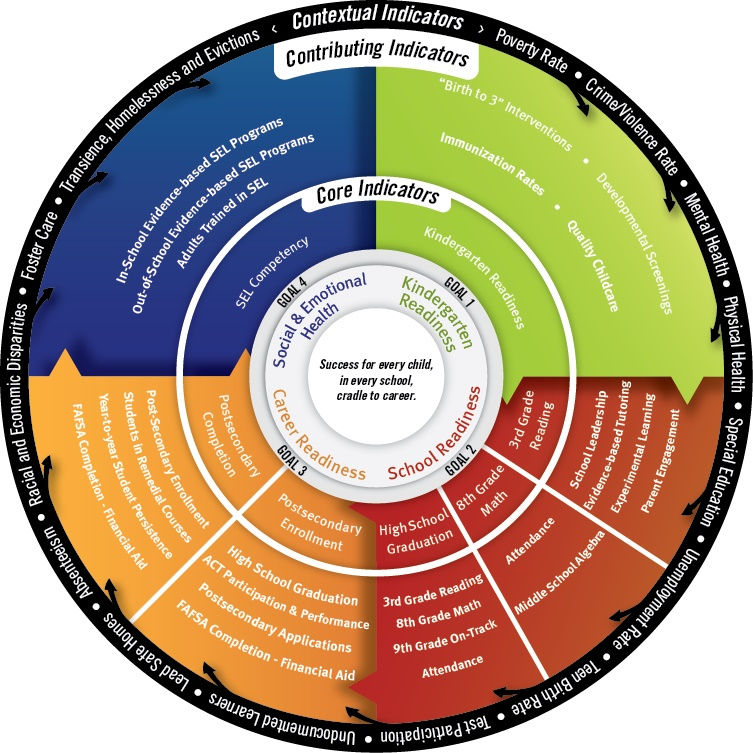
In Milwaukee, an example of developing common indicators to track can be found within the Milwaukee Succeeds project, one of 70 partnership projects in the StriveTogether Cradle to Career Network in the United States working to improve child outcomes. The work of Milwaukee Succeeds is aiming to improve educational indicators. A road map was developed collaboratively and seven core indicators (pictured below) as well as contributing indicators (many of which are health focused) were selected to track over time. This road map process is an excellent illustration of how existing data and new measures are taken together to track progress over time for community identified priorities.
Data & Analytic Resources
The Neighborhood Life Expectancy Project produces life expectancy estimates by census tract. The Virginia Commonwealth University also has life expectancy maps for several major United States Cities.
The County Health Rankings and Roadmaps website has a variety of tools, including data tables, data reports and mapping features, showing health outcome and measures data for geographic locations across the United States. Using the County Health Rankings data, users can enter a county and get a list of demographics, health outcome, health behaviors and social economic factors.
Community Commons provides a host of data on their website that can be mapped to different geographical units, many of which are more specific than county-level. For example, the Vulnerable Populations Footprint tool allows users to make a map of the area of interest and set thresholds for factors like poverty and educational attainment. The tools allows layering of data from discrete factors, helping to identify areas of potential vulnerability.
The National Equity Atlas stratifies economic data for geographic regions. In addition to providing data, the National Equity Atlas also suggests policies to address specific disparities that emerge through data analysis.
Other data mapping tools are the University of Wisconsin Neighborhood Atlas and the Annie E. Casey Kids Count Data Center.
Genesis Health Consulting has deep experience in partnering with health systems, foundations and communities to develop equity measurement strategies, indicators and analyze program impact on improving health equity. For more information, please contact us at info@genesishealthconsulting.com.





Comments